Inhalable Gene Therapy May Help Pulmonary Arterial Hypertension Patients
Gene therapy when inhaled may restore function of a crucial enzyme in the lungs to reverse deadly PAH.
The deadly condition known as pulmonary arterial hypertension (PAH), which afflicts up to 150,000 Americans each year, may be reversible by using an inhalable gene therapy, report an international team of researchers led by investigators at the Cardiovascular Research Center at Icahn School of Medicine at Mount Sinai.
In their new study, reported in the July 30 issue of the journal Circulation, scientists demonstrated that gene therapy administered through a nebulizer-like inhalation device can completely reverse PAH in rat models of the disease. In the lab, researchers also showed in pulmonary artery PAH patient tissue samples reduced expression of the SERCA2a, an enzyme critical for proper pumping of calcium in calcium compartments within the cells. SERCA2a gene therapy could be sought as a promising therapeutic intervention in PAH.
"The gene therapy could be delivered very easily to patients through simple inhalation — just like the way nebulizers work to treat asthma," says study co-senior investigator Roger J. Hajjar, MD, Director of the Cardiovascular Research Center and the Arthur & Janet C. Ross Professor of Medicine and Professor of Gene & Cell at Icahn School of Medicine at Mount Sinai. "We are excited about testing this therapy in PAH patients who are in critical need of intervention."
This same SERCA2a dysfunction also occurs in heart failure. This new study utilizes the same gene therapy currently being tested in patients to reverse congestive heart failure in a large phase III clinical trial in the United States and Europe.
"What we have shown is that gene therapy restores function of this crucial enzyme in diseased lungs," says Dr. Hajjar. "We are delighted with these new findings because it suggests that a gene therapy that is already showing great benefit in congestive heart failure patients may be able to help PAH patients who currently have no good treatment options — and are in critical need of a life sustaining therapy."
When SERCA2a is down-regulated, calcium stays longer in the cells than it should, and it induces pathways that lead to overgrowth of new and enlarged cells. According to researchers, the delivery of the SERCA2a gene produces SERCA2a enzymes, which helps both heart and lung cells restore their proper use of calcium.
"We are now on a path toward PAH patient clinical trials in the near future," says Dr. Hajjar, who developed the gene therapy approach. Studies in large animal models are now underway. SERCA2a gene therapy has already been approved by the National Institutes of Health for human study.
A Simple Inhalation Corrects Deadly Dysfunction
PAH most commonly results from heart failure in the left side of the heart or from a pulmonary embolism, when clots in the legs travel to the lungs and cause blockages. When the lung is damaged from these conditions, the tissue starts to quickly produce new and enlarged cells, which narrows pulmonary arteries. This increases the pressure inside them. The high pressure in these arteries resists the heart's effort to pump through them and the blood flow between the heart and lungs is reduced. The right side of the heart then must overcome the resistance and work harder to push the blood through the pulmonary arteries into the lungs. Over time, the right ventricle becomes thickened and enlarged and heart failure develops.
The gene therapy that Dr. Hajjar developed uses a modified adeno-associated viral-vector that is derived from a parvovirus. It works by introducing a healthy SERCA2a gene into cells, but this gene does not incorporate into a patient's chromosome, according to the study's lead author, Lahouaria Hadri, PhD, an Instructor of Medicine in Cardiology at Icahn School of Medicine at Mount Sinai.
"The clinical trials in congestive heart failure have shown already that the gene therapy is very safe," says Dr. Hadri. Between 40-50 percent of individuals have antecedent antibodies to the adeno-associated vectors, so potential patients need to be screened before gene therapy to make sure they are eligible to receive the vectors. In patients without antibodies, the restorative enzyme gene therapy does not cause an immune response, according to Dr. Hadri.
The clinical application of the gene therapy for patients with PAH will most likely differ from those with heart failure. The replacement gene needs to be injected through the coronary arteries of heart failure patients using catheters, while in PAH patients, the gene will need to be administered through inhalation.
This study was supported by National Institutes of Health grants (K01HL103176, K08111207, R01 HL078691, HL057263, HL071763, HL080498, HL083156, and R01 HL105301).
Other study co-authors include Razmig G. Kratlian, MD, Ludovic Benard, PhD, Kiyotake Ishikawa, MD, Jaume Aguero, MD, Dennis Ladage, MD, Irene C.Turnbull, MD, Erik Kohlbrenner, BA, Lifan Liang, MD, Jean-Sébastien Hulot, MD, PhD, and Yoshiaki Kawase, MD, from Icahn School of Medicine at Mount Sinai; Bradley A. Maron, MD and the study's co-senior author Jane A. Leopold, MD, from Brigham and Women's Hospital and Harvard Medical School in Boston, MA; Christophe Guignabert, PhD, from Hôpital Antoine-Béclère, Clamart, France; Peter Dorfmüller, MD, PhD, and Marc Humbert, MD, PhD, both of the Hôpital Antoine-Béclère and INSERM U999, Centre Chirurgical Marie-Lannelongue, Le Plessis-Robinson, France; Borja Ibanez, MD, from Fundación Centro Nacional de Investigaciones Cardiovasculares, Carlos III (CNIC), Madrid, Spain; and Krisztina Zsebo, PhD, of Celladon Corporation, San Diego, CA.
Dr. Hajjar and co-author Dr. Zsebo, have ownership interest in Celladon Corporation, which is developing AAV1.SERCA2a for the treatment of heart failure. Also, Dr. Hajjar and co-authors Dr. Kawase and Dr. Ladage hold intellectual property around SERCA2a gene transfer as a treatment modality for PAH. In addition, co-author Dr. Maron receives funding from Gilead Sciences, Inc. to study experimental pulmonary hypertension. Other study co-authors have no financial interests to declare.
About The Mount Sinai Medical Center
The Mount Sinai Medical Center encompasses both The Mount Sinai Hospital and Icahn School of Medicine at Mount Sinai. Established in 1968, the Icahn School of Medicine at Mount Sinai is one of the leading medical schools in the United States. The Icahn School of Medicine is noted for innovation in education, biomedical research, clinical care delivery, and local and global community service. It has more than 3,400 faculty members in 32 departments and 14 research institutes, and ranks among the top 20 medical schools both in National Institutes of Health (NIH) funding and by U.S. News & World Report.
The Mount Sinai Hospital, founded in 1852, is a 1,171-bed tertiary- and quaternary-care teaching facility and one of the nation's oldest, largest and most-respected voluntary hospitals. In 2012, U.S. News & World Report ranked The Mount Sinai Hospital 14th on its elite Honor Roll of the nation's top hospitals based on reputation, safety, and other patient-care factors. Mount Sinai is one of just 12 integrated academic medical centers whose medical school ranks among the top 20 in NIH funding and by U.S. News & World Report and whose hospital is on the U.S. News & World Report Honor Roll. Nearly 60,000 people were treated at Mount Sinai as inpatients last year, and approximately 560,000 outpatient visits took place.
For more information, visit http://www.mountsinai.org.
Find Mount Sinai on:
Facebook: http://www.facebook.com/mountsinainyc
Twitter @mountsinainyc
YouTube: http://www.youtube.com/mountsinainy
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
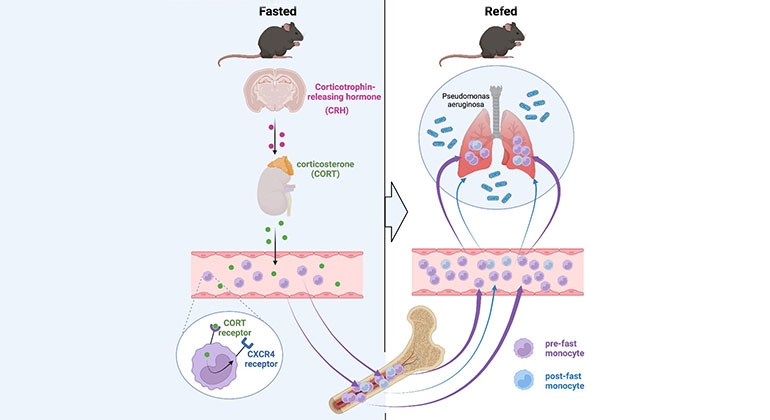
Skipping Breakfast May Compromise the Immune System
Feb 23, 2023 View All Press Releases
Valentin Fuster, MD, PhD, Named President of Mount Sinai Heart
Oct 18, 2022 View All Press Releases
.jpg)